African Marburg H-Fever
Deadlier than Ebola?
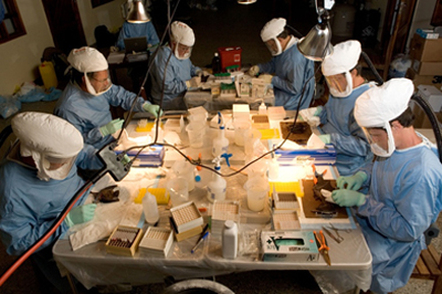 Bat-testing being done by a team of experts from CDC to determine the presence of Marburg H-fever virus. Image Centers for Disease Control
Bat-testing being done by a team of experts from CDC to determine the presence of Marburg H-fever virus. Image Centers for Disease Control
By Lino Cali Soriano
MARBURG Hemorrhagic Fever (or Marburg HF) once intensifies into a large-scale epidemic may become the ‘worst nightmare’ of health workers in Uganda and other parts of Africa primarily because there is no cure yet for this much-dreaded disease and it is highly transmissible.
In an email received by www.smartpinoysatbp.com from the Centers for Disease Control (CDC) in Atlanta, it was reported that this rare disease is a unique zoonotic (animal-borne but transmissible to humans) RNA virus of the filovirus family. The only known members of the filovirus are the five species of Ebola virus.
On October 6, 2014, the Uganda Health Ministry confirmed a single fatal case of Marburg HF. The patient is being treated at Mengo Hospital in Kampala. Investigation of the patient’s contact with family members and other persons is being conducted by the Uganda Virus Research Institute in collaboration with the CDC.
1967 Marburg HF Outbreak
In 1967, Marburg HF was first discovered after an outbreak of H-fever was simultaneously diagnosed in laboratories in Marburg and Frankfurt, Germany; in Belgrade, Yugoslavia, now Serbia. Here, 31 researchers and laboratory staff became ill, followed by several medical personnel and their family members who had cared for them. Of this number, seven deaths were reported. While conducting research, those who were first infected had been exposed to tissues and probably blood from imported green monkeys from Africa.
As of now, researchers from CDC are undertaking intensive research to determine if other species may also host the virus, aside from the reservoir host which is the African fruit bat (Rousettus aegyptiacus). This species of bat is widely scattered across Africa. Humans and other primates are susceptible to the Marburg virus and may develop serious disease with high rate of mortality.
Laboratory researchers confirmed that cases of Marburg HF had been reported in Uganda, Angola, Kenya, Zimbabwe, South Africa and the Democratic Republic of the Congo. Most of the victims started with nine male workers who were working in bat-infested mines. The virus is then transmitted within their respective communities by means of cultural practices and under-protected health care staff and family care settings.
In 1967 outbreak outside Africa occurred after a Dutch tourist developed Marburg HF after coming from Uganda and returning to the Netherlands. In 2008, a returning American tourist developed this disease after coming from Uganda, but he recovered. Both men had visited a popular cave inhabited by fruit bats.
CDC Report on the Marburg HF Transmission
“It is unknown how Marburg virus first transmits from its animal host to humans; however, for the 2 cases in tourists visiting Uganda in 2008, unprotected contact with infected bat feces or aerosols are the most likely routes of infection. After this initial crossover of virus from host animal to humans, transmission occurs through person-to-person contact. This may happen in several ways: direct contact to droplets of body fluids from infected persons, or contact with equipment and other objects contaminated with infectious blood or tissues.”
“In previous outbreaks, persons who have handled infected non-human primates or have come in direct contact with their fluids or cell cultures have become infected. Spread of the virus between humans has occurred in close environments and direct contacts. A common example is through caregivers in the home or in a hospital (nosocomial transmission).”
Signs and Symptoms The incubation period of Marbug HF is from 5-10 days, after which fever, chills, headache, and myalgia occur. On or about the fifth day after the onset of symptoms, a maculopapular rash, most prominent on the trunk (chest, back, stomach), may occur. Then may appear nausea, vomiting, chest pain, a sore throat, abdominal pain, and diarrhea. symptoms become progressively more pronounced and can include jaundice, inflammation of the pancreas, severe weight loss, delirium, shock, liver failure, massive hemorrhaging, and multi-organ dysfunction.
Clinical diagnosis of the disease can be tricky because many of symptoms of Marburg HF are similar to malaria, typhoid fever, or other infectious diseases. The problem is aggravated if it involves only a single case. CDC said that the case-fatality rate is between 23% and 90%.
Marburg HF can be prevented by people visiting Central Africa by avoiding fruit bats and sick nonhuman primates. While person-to-person transmission especially for health workers can be prevented by wearing CDC-recommended protective gowns, gloves and masks. Infected person must be placed in strict isolation, while needles, equipment and patient secretions must be properly disposed immediately. Treatment
CDC says, “There is no specific treatment for Marburg hemorrhagic fever. Supportive hospital therapy should be utilized, which includes balancing the patient's fluids and electrolytes, maintaining oxygen status and blood pressure, replacing lost blood and clotting factors, and treatment for any complicating infections.”
“Experimental treatments are validated in non-human primates models, but have never been tried in humans.”
For additional information visit www.cdc.gov
PLEASE PASS THIS ARTICLE TO OTHERS. THANKS.
Reference and Image: Centers for Disease Control and Prevention, Atlanta Georgia
MARBURG Hemorrhagic Fever (or Marburg HF) once intensifies into a large-scale epidemic may become the ‘worst nightmare’ of health workers in Uganda and other parts of Africa primarily because there is no cure yet for this much-dreaded disease and it is highly transmissible.
In an email received by www.smartpinoysatbp.com from the Centers for Disease Control (CDC) in Atlanta, it was reported that this rare disease is a unique zoonotic (animal-borne but transmissible to humans) RNA virus of the filovirus family. The only known members of the filovirus are the five species of Ebola virus.
On October 6, 2014, the Uganda Health Ministry confirmed a single fatal case of Marburg HF. The patient is being treated at Mengo Hospital in Kampala. Investigation of the patient’s contact with family members and other persons is being conducted by the Uganda Virus Research Institute in collaboration with the CDC.
1967 Marburg HF Outbreak
In 1967, Marburg HF was first discovered after an outbreak of H-fever was simultaneously diagnosed in laboratories in Marburg and Frankfurt, Germany; in Belgrade, Yugoslavia, now Serbia. Here, 31 researchers and laboratory staff became ill, followed by several medical personnel and their family members who had cared for them. Of this number, seven deaths were reported. While conducting research, those who were first infected had been exposed to tissues and probably blood from imported green monkeys from Africa.
As of now, researchers from CDC are undertaking intensive research to determine if other species may also host the virus, aside from the reservoir host which is the African fruit bat (Rousettus aegyptiacus). This species of bat is widely scattered across Africa. Humans and other primates are susceptible to the Marburg virus and may develop serious disease with high rate of mortality.
Laboratory researchers confirmed that cases of Marburg HF had been reported in Uganda, Angola, Kenya, Zimbabwe, South Africa and the Democratic Republic of the Congo. Most of the victims started with nine male workers who were working in bat-infested mines. The virus is then transmitted within their respective communities by means of cultural practices and under-protected health care staff and family care settings.
In 1967 outbreak outside Africa occurred after a Dutch tourist developed Marburg HF after coming from Uganda and returning to the Netherlands. In 2008, a returning American tourist developed this disease after coming from Uganda, but he recovered. Both men had visited a popular cave inhabited by fruit bats.
CDC Report on the Marburg HF Transmission
“It is unknown how Marburg virus first transmits from its animal host to humans; however, for the 2 cases in tourists visiting Uganda in 2008, unprotected contact with infected bat feces or aerosols are the most likely routes of infection. After this initial crossover of virus from host animal to humans, transmission occurs through person-to-person contact. This may happen in several ways: direct contact to droplets of body fluids from infected persons, or contact with equipment and other objects contaminated with infectious blood or tissues.”
“In previous outbreaks, persons who have handled infected non-human primates or have come in direct contact with their fluids or cell cultures have become infected. Spread of the virus between humans has occurred in close environments and direct contacts. A common example is through caregivers in the home or in a hospital (nosocomial transmission).”
Signs and Symptoms The incubation period of Marbug HF is from 5-10 days, after which fever, chills, headache, and myalgia occur. On or about the fifth day after the onset of symptoms, a maculopapular rash, most prominent on the trunk (chest, back, stomach), may occur. Then may appear nausea, vomiting, chest pain, a sore throat, abdominal pain, and diarrhea. symptoms become progressively more pronounced and can include jaundice, inflammation of the pancreas, severe weight loss, delirium, shock, liver failure, massive hemorrhaging, and multi-organ dysfunction.
Clinical diagnosis of the disease can be tricky because many of symptoms of Marburg HF are similar to malaria, typhoid fever, or other infectious diseases. The problem is aggravated if it involves only a single case. CDC said that the case-fatality rate is between 23% and 90%.
Marburg HF can be prevented by people visiting Central Africa by avoiding fruit bats and sick nonhuman primates. While person-to-person transmission especially for health workers can be prevented by wearing CDC-recommended protective gowns, gloves and masks. Infected person must be placed in strict isolation, while needles, equipment and patient secretions must be properly disposed immediately. Treatment
CDC says, “There is no specific treatment for Marburg hemorrhagic fever. Supportive hospital therapy should be utilized, which includes balancing the patient's fluids and electrolytes, maintaining oxygen status and blood pressure, replacing lost blood and clotting factors, and treatment for any complicating infections.”
“Experimental treatments are validated in non-human primates models, but have never been tried in humans.”
For additional information visit www.cdc.gov
PLEASE PASS THIS ARTICLE TO OTHERS. THANKS.
Reference and Image: Centers for Disease Control and Prevention, Atlanta Georgia

